Quick Links
For Patients

© Copyright 2026 American TelePhysicians. All rights reserved.



A direct relationship between hip fractures in the United States population and age has been established. Furthermore, fractures and hip pain are usually seen in older demographics in the US and everywhere globally.
Every year 300,000 people are hospitalized for hip-related trauma (predominantly fractures), and over 60% of hospital admissions are of people over 65. In addition, older women are more likely to complain of hip (and other osteologic) complaints.
The underlying cause of hip pain can vary from direct and indirect trauma to tumors and infections. Therefore, a physician must make a correct assessment of what's causing the pain and deduce a treatment plan for relieving it. Any delays in formulating an appropriate treatment plan can lead to dire consequences.
For example, arthritis caught on early can be managed or relieved with appropriate rehabilitation and medications. Surgeries might become necessary, however, if the diagnosis is incorrect because of improper imaging.
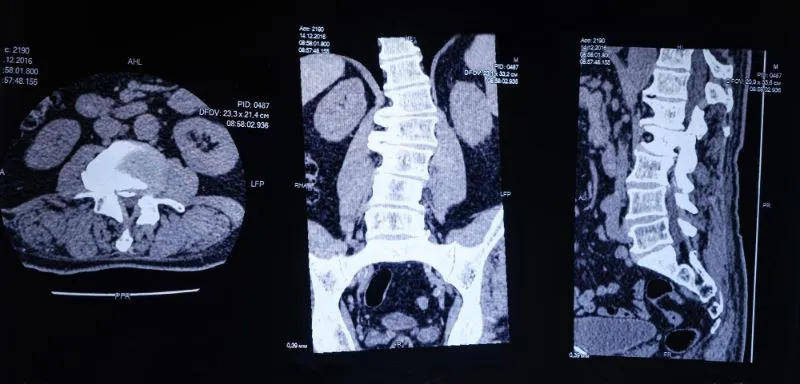
Radiology refers to the branch of medicine that deals with imaging internal bodily functioning and systems. Hip, For example, imaging is instrumental in diagnosing pathologies and traumas to the ilium, sacrum, lumbar spine, associated muscles, and soft tissues.
Multiple images of the hip are necessary for a correct diagnosis and for creating an adequate treatment plan. This includes:
Magnetic Resonance Imaging (MRI) is one of the most sensitive tests for examining and diagnosing bone and surrounding soft tissues. In addition, MRI tests can detect stress fractures, mild tissue trauma, and infections.
Osteoarthritis is a complicated condition of multi-factorial origin. The underlying characteristic is the breakdown of the hyaline cartilage along articulating joints. The epidemiology is usually in older demographics (typical women after menopause).
Diagnosing osteoarthritis is often done via radiographs and imaging modalities such as MRIs and X-rays. These techniques are non-invasive (unless contrast dyes are used) because of their low costs, quick results, and accuracy. An MRI is considered the gold standard for hip OA between MRIs and radiographs since articular cartilage is visible and has a much higher resolution of surrounding tissues. Multiple criteria are used for OA, including numerous clinical prediction rules incorporating limited hip internal rotation, hip pain with specific activities, and stiffness in the morning for sixty minutes or less.
An MRI is a good tool for evaluating the many causes of pain that may surround the hip joint itself. For example, several tendons inserted around the hip can become inflamed or degenerated. Likewise, bursitis can be painful, usually located at the hip's outside (lateral) part. In addition, if you have had a recent injury or engaged in excessive athletic activity, your muscles can become injured (known as a "muscle strain"), and an MRI can detect this.
An MRI often shows unexpected causes of hip pain originating from other nearby structures like the sacroiliac joints, pubic bones, or even the lower lumbar spine.
More worrisome sources of pain that could be coming from tumors, infection, or necrosis of the bone (also known as AVN) can also be eliminated from the list of potential causes by doing an MRI. MRI evaluates some of these causes with intravenous contrast.
The average expense of an MRI in the United States is $1,325. However, costs can go from $375 to $2,850. One factor that can significantly influence the expense of an MRI is whether your insurance covers it. The payment for an MRI will be higher if you don't have medical coverage.
Another significant component that can extraordinarily influence the expense of an MRI is whether you have an in-patient office, similar to a medical clinic, or an outpatient medical procedure community. Outpatient clinics save you thousands on your hospital bill.
Different locations charge differently:
Your physician would recommend an MRI for the hip if they suspect an underlying pathology inconsistent with the initial diagnosis. Likewise, if they suspect a tumor or an infection that can be dangerous or deadly.
You'll have cause to visit your regular care physician if the swelling doesn't go down, bleeding is uncontrollable, or you experience pain for longer than a reasonable time frame.
Our clinical experts continually monitor the health and medical content posted on CURA4U, and we update our blogs and articles when new information becomes available. Last reviewed by Dr. Tayyab S. Akhtar on May 11th, 2023.

Sirpa Talvikki Autio MD


Please note that these services are not intended for any emergency medical situations. If you are having a life-threatening or serious condition that may require hospitalization, including, but not limited to, high-grade fever; low or high blood pressure; active serious infection, including, but not limited to, COVID; chest pain; shortness of breath; severe pain; or stroke-like symptoms, please call 911 immediately or go to a nearby emergency center as quickly as possible.
If you do not have a physician's order for labs or non-invasive radiology services, you may request it through our network of affiliated physicians/providers in selected states for an additional non-refundable fee, as listed (asynchronous consultation). Please note that an asynchronous consultation or physician-order service for diagnostics is not available for radiology tests requiring IV contrast. Patients needing a diagnostic study with IV contrast must complete an online visit with our physician first and, likely, will also need to have a lab test for their kidney function before a diagnostic study with IV contrast can be scheduled.
Once you request our provider or physician's order service, you will receive an email from us inquiring more details about your medical history. Based on the information you provide, one of our affiliated physicians or providers will make a determination about processing the order for the requested service. In some cases, as determined by our affiliated medical team, you may be required to provide additional clinical information or may be asked to have a more detailed online visit (an additional fee may apply) before your order can be processed. Please note that in some situations, or based on available clinical information, our team may even decide not to process the requested diagnostic order service and rather may recommend you to seek immediate medical attention in person or go to the nearest urgent care or ER. In that case, any advanced payment for the diagnostic service(s) will be refunded, but the physician's consultation or order request fee will remain non-refundable.
Please also note that any post-diagnostic service follow-up visit(s) or treatment(s) is not covered in this service fee and the ordering physician is not responsible to provide any continued care unless you sign-up for that service separately. Depending on your situation or test results, you may be advised to seek consultation with either primary care or a specialist physician (local or online) for further work-up and treatment. If you are unsure or have any questions, please call our customer support service before placing an order.
By clicking "Continue", you agree to the policy, terms, and conditions.